Are We Ready?
By Dr. Mary Sproull, Research scientist, National Cancer Institute – National Institutes of Health, USA.
Since the events of 9/11, we have come a long way in terms of preparedness for future CBRNe events. Perhaps the greatest successes have been in development of preparedness guidelines and medical countermeasures for emergencies involving radiological or nuclear threats. Though we have now accumulated a solid foundation of resources for operational management of these events, there remain key areas of mass casualty emergency planning that have yet to be fully addressed.
Prior to 9/11, the world of civil defense for radiological or nuclear event scenarios had stalled with the “duck and cover” public education initiatives of the Cold War era. With the advent of global terrorism, initiatives were undertaken to develop:
- Modern operational guidelines for future large scale radiological or nuclear event scenarios and with the support of legislation which established Project Bioshield.
- Concurrent procurement and licensure of medical countermeasures specific for radiation injury.
Medical countermeasures tackling radiological and nuclear threats
We now have extensive playbooks developed at the federal level detailing emergency planning and response guidelines for these event scenarios, with guidelines specific to threats involving radiological dispersal devices or nuclear events. We also have several medical countermeasures recently approved by the FDA for treatment of radiation injury including filgrastim (Neupogen®), pegfilgrastim (Neulasta®), sargramostim (Leukine®), and romiplostim (Nplate®).
These drugs can be used to treat the hematopoietic sub-syndrome of the acute radiation syndrome (H-ARS), which is caused by the myelosuppressive effects of radiation exposure. In addition, the FDA has just recently cleared Silverlon® for use in treatment of cutaneous radiation injury (burns) and radiation dermatitis. These drugs represent a significant cadre of frontline medical countermeasures that physicians can use to treat the early stages of acute radiation injury.
Other key medical countermeasures in development include blood diagnostics to determine level of radiation exposure using biodosimetry algorithms. Select biodosimetry assays using proteomic or genomic approaches are in late-stage development for FDA licensure and expected to be added to the Strategic National Stockpile. These blood tests are designed to be either point-of-care with field deployment capability or high-throughput, processed at off-site labs as a reach-back resource. More efficient cytogenetic biodosimetry assays and inter-laboratory standardization efforts are also in development to create additional reach-back surge capability.
Biodosimetry diagnostics remain a key medical resource, critical to the successful implementation of existing emergency preparedness plans, as they are the “lynchpin” of effective mass casualty medical management of future events involving radiation exposure. Preliminary screening to identify the level of received radiation dose is critical for efficient triage and allocation of scarce medical resources, such as the afore mentioned drugs for radiation exposure.
Screening to separate who has been exposed from who has not is also critical to alleviate the burden of the “worried well” or “concerned citizens” on the existing medical systems. Based on historical precedence, these uninjured or walking wounded persons, who want to know if they have been exposed to radiation, are expected to overwhelm local medical resources.
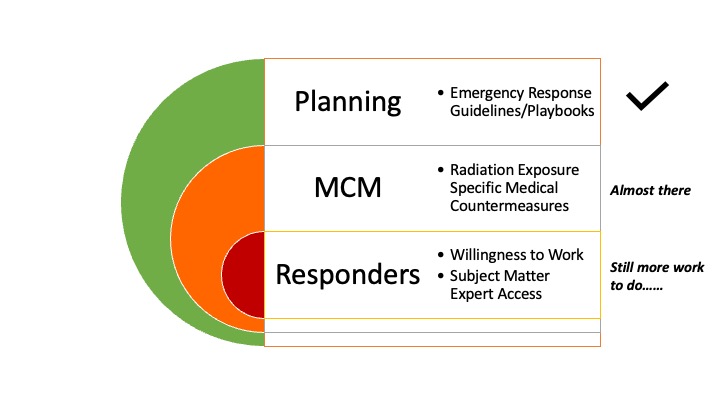
Building operational readiness is challenging
Therefore, diagnostics to reassure these persons and to determine the degree of exposure more effectively for radiation specific triage are needed. Emergency planning efforts at the federal level are also supplemented by the work of organizations like the National Alliance for Radiation Readiness (NARR), the Radiation Injury Treatment Network (RITN) and the National Association of County and City Health Officials (NACCHO) to promote training and operational readiness for emergencies involving radiation threats at the state and local level in the U.S.
One critical aspect of emergency planning for future scenarios involving radiological hazards is social behavior. Radiation exposure, and all of the CBRN family of threats, fall into the social phenomena class of “dreaded risks” which evoke a disproportionate fear of the risk compared to the actual health impact.
The observation that this extreme fear of radiation exposure exists ubiquitously throughout society has led some emergency planners to postulate that “willingness to work,” (WTW) or the willingness of first responders and hospital workers to show up to work in situations where there are radiological hazards present, might represent a large confounder to emergency planning. Survey studies of numerous populations of first responders, physicians, and general hospital staff have indicated that fear of radiation exposure will impact WTW for future radiological emergencies.
Current planning documents and concepts of operations (CONOPs) for future radiological or nuclear event scenarios do not take this potential social confounder into consideration.

Science attempts to bring solutions
Work is being done at George Mason University’s Center for Social Complexity using computational modeling to simulate movement and social interaction of populations under such circumstances. Currently they are modeling “Human-Infrastructure Interactions Following Nuclear Detonations” as part of the Defense Threat Reduction Agencies’ Social Impacts of Nuclear Detonations (SIND) program to examine physiological (i.e., injuries or casualties from nuclear detonations), psychological, and sociological phenomena/behaviors.
Another recent computational model study completed through the Center, “Modeling of Mass Casualty Management During a Radiological or Nuclear Event” explored the role of communication and information flow between first responders and radiation subject matter experts (SMEs) and found that WTW amongst first responders increased with the presence and improved communication access to radiation SME in the field. This model of social interaction suggested that the presence of radiation SME and prioritizing communication access for SME over other general emergency response personnel was key to mitigating radiation dread.
Work is currently underway to certify more radiation SME, in the form of the Radiological Operations Support Specialist (ROSS) program supported by the Federal Emergency Management Agency, which seeks to recruit and train radiation health professionals within local communities for deployment/support during future radiological or nuclear events.
“Increased funding to support training of first responders and medical personal themselves on the relative health risks of radiation exposure is needed”
There is room for improvement
As primary response for any emergency is initially a local response, development of a base of local radiation experts nationwide is an important step for civil defense. Integration and establishment of working relationships between these local radiation SME and the first responders and medical professionals they will be supporting prior to future emergencies is also key to ensure a level of trust for effective mitigation of radiation dread. The ROSS program is an important aspect of emergency preparedness which should receive more visibility, financial support, and resources to increase access for training opportunities at the local level. Further, increased funding to support training of first responders and medical personal themselves on the relative health risks of radiation exposure is needed.
We have come a long way towards operational readiness for a future nuclear or large-scale radiological event. We have comprehensive playbooks for emergency preparedness and response utilizing deployment of national resources with support from agencies across the federal landscape. We have a cohort of medical countermeasures specific to radiation injury licensed and stockpiled.

In areas related to medical management we need continued effort to develop additional surge capacity for burn treatment at the national level, licensure of field ready biodosimetry diagnostics and of additional medical countermeasures specific to the other sub-syndromes of the ARS including the gastrointestinal and neurovascular syndromes.
We also need to address the phenomena of WTW in first responders specifically for radiological or nuclear event scenarios. The phenomenal amount of effort over the last decade which has been invested in development of CONOP’s and radiation exposure specific medical countermeasures will be futile if no one shows up to work. Research into mitigation strategies for alleviating perception of risk in first responders is essential. Increased funding and access for local first responders and hospital personnel for training on radiation specific hazards and education on radiation related health risks, as well as access to local radiation SME, are critical remaining steps towards ensuring we have the manpower to support and implement our existing response systems. We have come a long way towards true national readiness for a large-scale radiation emergency but still have a bit further to go.
*These comments represent the work and opinions of the author and do not constitute official positions of the National Institutes of Health (NIH) or the U.S. Department of Health & Human Services (HHS). References to any specific commercial products by the trade name, trademark, manufacturer or otherwise, does not necessarily constitute or imply its endorsement, recommendation, or favoring by NIH or HHS.
About the Author:
Mary Sproull, PhD is a research scientist in the Radiation Oncology Branch of the National Cancer Institute at the National Institutes of Health. Her current work at the National Institutes of Health is funded by the Radiation and Nuclear Countermeasures Program/National Institute of Allergy and Infectious Diseases, as part of an initiative to develop new radiation biodosimetry models for dose prediction for use during mass casualty management during a radiological or nuclear event.



